If you or a loved one have suffered from a stroke, it is difficult to come to terms with the health implications that affect daily life. Upper limb deficit after stroke, especially, causes stroke survivors to need help in daily tasks. Recovery is a long, arduous path.
In the past, physical therapists have been able to develop techniques to help stroke survivors. In turn, they can regain mobility and function as well as speech. Not everyone has been able to fully recover, but scientists are working on advanced treatments every day.
The newest, most groundbreaking stroke technology is called "Vivistim." Vivistim uses the science of electrical stimulation and applies it to what doctors understand about strokes.
If you're wondering if vivistim is an option for you or a loved one, read this guide.
Strokes - First Let's Understand What They Are
A stroke is an interruption or reduction to the blood supply to your brain. As such, brain cells can alter and die leaving paralyzing outcomes as the loss of blood flow to the brain damages brain tissue. There are many instances where a person may not realize they are having a stroke so it's important to know what the symptoms are in order to seek emergency medical attention or someone in need.
How Does Vivistim Work?
In general, people understand that strokes happen in the brain and affect our ability to move the rest of our body. What they don't understand is exactly what happens and how we lose control of our bodily functions. To understand vivistim, you need a deeper education on strokes.
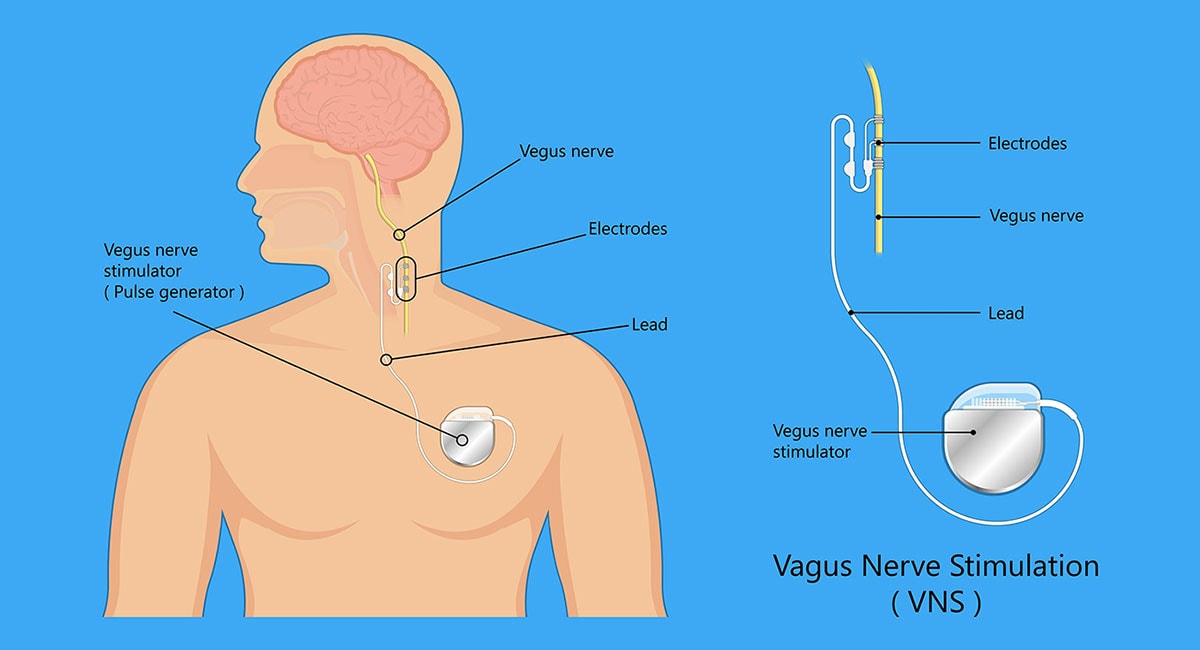
The Vagus Nerve
The vagus nerve is arguably the most important nerve that extends from our brain to our body. We have twelve cranial nerves, or nerves that come from the brain, all of which transfer information from our brain to our organs and tissues.
The vagus nerve's four key functions are sensory, special sensory, motor, and parasympathetic.
The sensory category of the vagus nerve function covers our throat, heart, abdomen, and lungs. The special sensory covers the taste in the back of our tongue. The motor helps us move the muscles needed for swallowing and speech, while the parasympathetic helps us with digestive, respirative, and cardiac functions.
In conclusion, the vagus nerve helps us relax, digest, lower inflammation and blood pressure, and even control fear. When we suffer from a stroke, many of these functions provided by the vagus nerve can't work properly. Vivistim uses the power of the vagus nerve to help us regain control of our bodily functions.
Electrical Signals and Our Brain
Our brains communicate through electrical signals which travel through nerves and out to our tissues and organs. These electrical signals tell the rest of our body what to do and how it should act. If a stroke disrupts these electrical signals, the brain can no longer communicate with the body.
The organs and tissues also interact with nerves to send signals back to the brain. In this way, the brain and body can communicate and the brain can monitor bodily functions.
In the same way that our brains send out electrical signals to communicate, we can send electrical signals to the brain to cause certain reactions. Vivistim takes advantage of this electrical communication method and the vagus nerve to help our brain communicate again.
Vivistim Therapy
Vagus nerve stimulation (VNS) has been used successfully for years to treat other conditions, most notably epilepsy. However, the vivistim system goes beyond vagus nerve stimulation. It uses VNS during rehabilitation exercises to help stroke victims regain motor function in their upper limbs.
The vivistim system works with an implant and a physical therapist. A doctor implants a vivistim implant on the vagus nerve in the stroke survivor. A physical therapist can tell the implant to send electrical signals through the vagus nerve to the brain.
These signals get sent through the Nucleus Tractus solitarius (NTS) and hit two distinct regions of the brain. When these signals meet the brain, they stimulate the release of neurotransmitters across the brain. The neuromodulators, or brain chemicals, help strengthen the exercise because they are important for memory and learning.
In addition, by stimulating the brain with neurotransmitters, a doctor can improve neuroplasticity and thereby increase motor function in the patient.
This therapy, however, is not as simple as just sending signals to the brain. Doctors and patients must work together to make sure the signal's pulse is in correlation with positive motor functions. In doing this, a therapist can retrain the brain to behave the way it did before the stroke.
Electrical stimulation sent during a rehabilitative exercise alerts the brain to that specific movement. Consistently working on these exercises paired with VNS helps rebuild neural circuits for those specific movements. In addition, this vivistim system can help rebuild muscles that have become weak due to lack of use.
Over time, the vivistim system can result in a patient's ability to use their limbs again.
What Does the Vivistim System Look Like?
If you need a visual example, picture a stroke victim and a physical therapist sitting in a room. The physical therapist is sitting behind their computer, which connects to both a control button and a wireless transmitter. The wireless transmitter communicates with the implant inside of the patient.
The physical therapist can instruct the patient to attempt a simple movement with the afflicted limbs. For example, maybe they must pick up a cup from the table. While the patient is attempting the exercise, the physical therapist will push the button so that the implant sends out an electrical pulse.
Doing these exercises repeatedly with this non-invasive nerve stimulation will help the stroke patient's brain to recognize the movement and eventually be able to cause those movements fully on its own again.
What Is the Vivistim Implant Like?
Before you have a medical device implanted in your body, it's likely that you'll want to know what it looks like and where it goes.
A vivistim system consists of four different technological parts:
- Pulse generator
- VNS lead
- Stroke Application and Programming Software (SAPS)
- Wireless transmitter
The first two parts, the pulse generator and the lead, make up the medical device that goes inside your body. The last two parts, the software and the transmitter, are the parts controlled by the physical therapist.
The pulse generator is a little box powered by a battery. It is less than 70 grams and puts out a frequency between 1 and 30 Hz. The physical therapist will start sending pulses on the lowest level and increase until the right level of the pulse is showing results.
The lead is a 43 cm long silicone wire. One end inputs into the pulse generator. The other end has a cuff that is attached to your vagus nerve. The pulse generator receives the signals from the physical therapist and sends the electrical pulse down the lead to the vagus nerve.
The software is easily downloaded by a physical therapist on their laptop and connects with push-button control. The wireless transmitter specifically made for the vivistim system is connected to the laptop so that it can take commands from the software.
How Long Does the VNS Implant Last?
VNS implants have been used for years on epilepsy patients. These implants have a battery that lasts about ten years. Your doctor will schedule a surgery similar to the one used to implant the device so they can change the battery.
VNS implants might not work when you are too close to a magnetic device or field. If the implant is not working, your physical therapist should check your surroundings and ask if you have anything magnetic on your person that could interrupt the device's function.
VNS Side Effects
While VNS side effects are rare and subtle, there are a few to be aware of. People who have a VNS implant may experience discomfort while the device is in use. These side effects could include throat discomfort, difficulty swallowing, coughing, and a hoarse voice.
It's possible that side effects will lessen over time as your body gets used to the stimulation. If they are bad enough, a physical therapist will know to hold up a magnet to the device to interrupt the signal.
VNS implants do not interact at all with other drugs, so it is a safe therapy to use while taking medications.
On the other hand, VNS has been known to produce many beneficial effects. Users have reported elevated moods and improved memory. They've also reported feeling more alert and reducing depression.
Is Vivistim Available through My Provincial Insurance Plan?
VNS therapy is currently fairly expensive, as it requires both surgery and continued therapy sessions. On average, VNS therapy can cost a little over $25,000 without insurance. In Canada, there are set medical conditions that can be considered valid reasons to receive VNS therapy.
Currently, four hospitals in Ontario provide VNS implantation surgeries at no cost when done for epilepsy or treatment-resistant depression. If you are covered by OHIP, you can receive continued VNS therapy at 6 different centers.
However, VNS therapy for stroke patients is very new and therefore is still undergoing trials. The therapy is still considered experimental. Therefore, it might be a while before it is covered by insurance plans.
Since there is approval for VNS therapy for other health conditions, however, there is hope that insurance policies will soon cover the therapy for strokes.
Learn More About Health and Insurance Plans
If you are trying to plan out your health and find treatments, especially vivistim, knowing what's covered on your provincial insurance plan is crucial. Insurdinary is a great resource for learning about medical treatments and how your insurance can affect the costs.
If you're looking to compare insurance plans or learn more about your own, visit Insurdinary's comprehensive guide on provincial insurance plans!